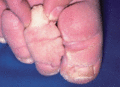
Figure 105.1
The Kaposi–Stemmer sign: an inability to pinch or pick up a fold of skin at the base of the second toe indicates lymphoedema.

Figure 105.5
Acute and chronic lipodermatosclerosis; the bright red skin (acute) could be mistaken for bacterial cellulitis but it is an inflammatory response to t...

Figure 105.9
Solid facial oedema.
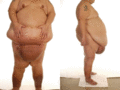
Figure 105.13
Lymphoedema of the pendulous abdomen and mons pubis from obesity.
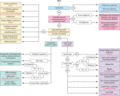
Figure 105.17
Classification pathway for primary lymphoedema. Text in red indicates the suggested genetic test for the subgroup. Please refer to Table for the def...
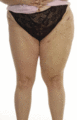
Figure 105.21
Atruncular lymphatic malformation without lymphoedema.
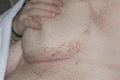
Figure 105.25
Benign lymphangiomatous papules (atypical vascular lesions) post radiotherapy.
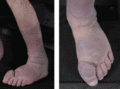
Figure 105.29
Pretibial myxoedema.
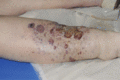
Figure 105.33
Lymphangiosarcoma arising in primary lymphoedema.
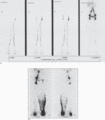
Figure 105.2
(a) Normal lymphoscintigraphy. Images show patent lymph routes draining tracer from the feet to the ilio‐inguinal nodes. (Courtesy of Professor A. M....
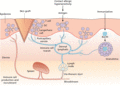
Figure 105.6
The lymphatic vessel sits centre stage for immune cell trafficking within the skin. DC, dendritic cell. (From Mortimer et al. 2014 [ ].)
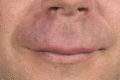
Figure 105.10
Oro‐facial granulomatosis exhibiting redness and indurated swelling of the right upper lip.
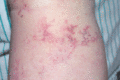
Figure 105.14
Carcinoma erysipeloides (carcinoma telangiectatica): the red vessels are dermal lymphatic vessels infiltrated with adenocarcinoma of the breast.
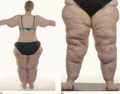
Figure 105.18
A patient with classic lipoedema. (a) Symmetrical fatty swelling of both lower limbs with sparing of the trunk. Increased adipose deposition of the up...
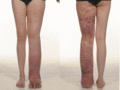
Figure 105.22
Truncular lymphatic malformation with blood‐filled cutaneous lymphangiectasia and lymphoedema.

Figure 105.26
Vulval lymphangiectasia showing acquired lymphangiomas (lymphangiectasias) following cervical cancer treatment. The lymphangiomas were mistaken for g...
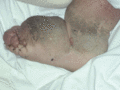
Figure 105.30
Elephantiasis verrucosis nostras showing marked hyperkeratosis and papillomatosis.
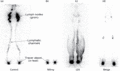
Figure 105.34
Lymphoscintigraphs showing the uptake of technetium‐99 in the inguinal lymph nodes (ILNs) at 2 h after injection in the normal lymphatic system and in...
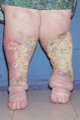
Figure 105.3
Lymphoedema associated with chronic venous disease.
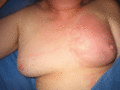
Figure 105.7
Recurrent cellulitis in lymphoedema following breast cancer treatment. Note lymphangitis crossing the watershed to the contralateral lymph node territ...
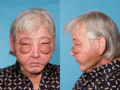
Figure 105.11
Severe facial lymphoedema following treatment for carcinoma of the tongue.
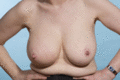
Figure 105.15
Breast lymphoedema following cancer treatment. Note pitting from bra indentations in the skin of the right breast.
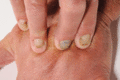
Figure 105.19
Yellow nail syndrome showing slow‐growing, overcurved, thickened nail plates and hand oedema.
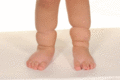
Figure 105.23
Amniotic bands and lymphoedema.
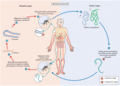
Figure 105.27
The life cycle of filarial nematodes in the human and mosquito hosts. Wuchereria bancrofti, Brugia malayi and B. timori have similar life cycles. ...
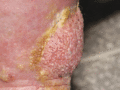
Figure 105.31
Acquired cutaneous lymphangiectasia leading to ulceration of the lower leg.
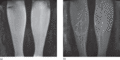
Figure 105.35
(a) Baseline magnetic resonance lymphangiography (MRL) images taken from a patient prior to contrast injection. His phenotype is of lymphoedema distic...
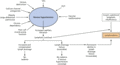
Figure 105.4
Causes of mixed lymphovenous disease and phlebolymphoedema.
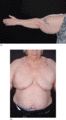
Figure 105.8
Madelung disorder. (a) Benign symmetrical lipomatosis (also known as benign symmetrical lipomatosis of Launois–Bensaude, Madelung disease, multiple sy...
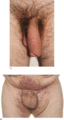
Figure 105.12
(a) Lymphoedema of the penis secondary to ano‐genital granulomatosis. There may be no sign of inflammation. (b) Genital lymphoedema secondary to hidra...
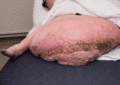
Figure 105.16
Massive localized lymphedema of the right thigh showing marked ‘cobblestone’ skin changes.
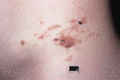
Figure 105.20
Lymphangioma circumscriptum showing fluid‐filled vesicles resembling frogspawn. At times the vesicles can contain blood, weep clear fluid (lymphorrhoe...
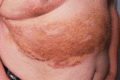
Figure 105.24
Kaposiform lymphangiomatosis showing a Kaposi sarcoma‐like rash with localized lymphoedema of the breast and chest wall associated with haemoptysis.
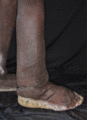
Figure 105.28
Lower limb lymphoedema due to podoconiosis. Note the presence of toe maceration and typical ‘mossy’ appearance of the foot. (Reproduced with permissi...
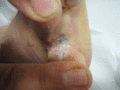
Figure 105.32
Macerated web‐space skin leads to bacterial entry points and fungal infection.

Figure 105.36
(a) Toe (or finger) bandaging with cotton crepe bandages. (b) Sub‐bandage wadding over a tubular cotton bandage. (c) Short‐stretch compression cotton ...

